FEATURED EMPLOYEE BENEFITS CASE STUDY
FEATURED CASE STUDY
ABOUT THE CLIENT
A healthcare facility with nursing homes in 18 locations spread out over Texas, Louisiana and Arkansas. This client employs more than 1,800 employees.
THE CHALLENGE
Before AGM was involved, the client had a very hard time communicating benefits and enrolling employees on paper. Open enrollment wasn’t the only challenge. The HR department was spread thin and having a hard time keeping up with mid year employee changes, terminations and billing reconciliation. The client realized they needed an experienced benefits enrollment partner, to streamline employee benefits communication, enrollment and administration.
THE CHALLENGE
Before AGM was involved the client had a very hard time communicating benefits and enrolling employees on paper. Open enrollment wasn’t the only challenge. The HR department was spread thin and having a hard time keeping up with mid year employee changes, terminations and billing reconciliation. The client realized they needed an experienced benefits enrollment partner, to streamline employee benefits communication, enrollment and administration.
OPEN ENROLLMENT OBJECTIVES
Active Enrollment: All employees were required to attend.
Enrollment: Salary based counselor assisted laptop enrollment.
Benefits Marketing Material: Create a custom benefit guide that simplified benefit options.
Call Center: Establish a dedicated 1-800 # for employees to utilize for open enrollment, new hire enrollment, and all customer service calls.
Consolidate Voluntary Carriers: Consolidating 3 voluntary carriers to 1.
Education: On-site communication and education of benefit plans.
Census Data: Update employee demographic records, beneficiaries, spouse and dependent information.
Benefits Technology: Implement a benefits administration platform to move away from paper enrollment and administration.
OPEN ENROLLMENT OBJECTIVES
Active Enrollment: All employees were required to attend.
Benefits Marketing Material: Create a custom benefit guide that simplified benefit options and clearly explained what is available.
Enrollment: Salary based counselor assisted laptop enrollment.
Call Center: Establish a dedication 1-800 # for employees to utilize for open enrollment, new hire enrollment, and all customer service calls.
Consolidate Voluntary Carriers: Consolidating 3 voluntary carriers to 1.
Census Data: Update employee demographic records, beneficiaries, spouse and dependent information.
Education: On-site communication and education of benefit plans.
Benefits Technology: Implement a benefits administration platform to move away from paper enrollment and administration.
PROVEN RESULTS
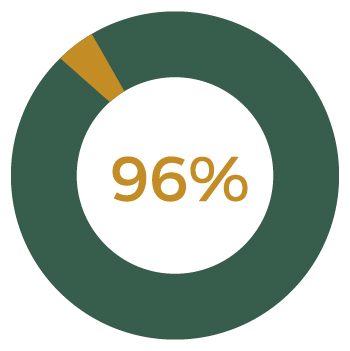
96% of employees completed their enrollment on-site with an enrollment counselor or by phone through the AGM Benefit Enrollment Call Center.

A custom employee benefits booklet was designed and distributed to all employees for the first time ever.
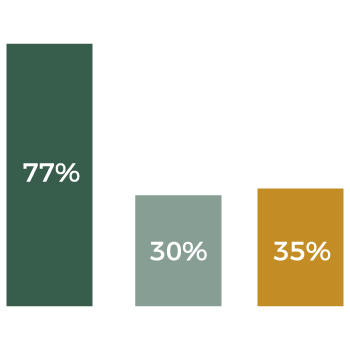
• 77% of employees enrolled in the new voluntary worksite benefit plans.
• Dental, vision, and long term disability participation increased by 30%
• HDHP participation increased by 35%

AGM received a 98% satisfaction rating on a post enrollment survey sent to employees.